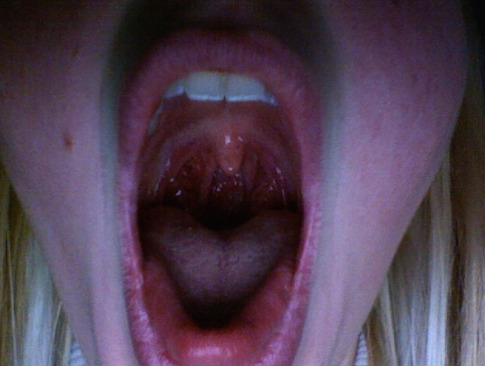
This week we take a look at a rare vocal disorder called Spasmodic Dysphonia. It can greatly effect your vocal cords, resulting in a strangled-sounding or hoarse voice. For some, it seems like they have lost their voice. It can be treated with a combination of speech therapy and Botox, but there is currently no cure.
My name is Mark and I am 36 years old. I have always relied heavily on my communication and people skills to get me ahead of everybody else. I never would have thought that I would struggle with something everybody takes for granted.
I can’t pinpoint the exact moment where my life changed but I know for a fact that it happened in early 2006 while I was working for the San Antonio Express News in their call center as a Customer Service Representative. I was struggling to speak and was hesitating with certain words and phrases. It was extremely embarrassing!
I kept asking myself: Why is this happening? Will it ever go away? Will I lose my voice? Could it be stress related? Is it psychological?
There were certain words and letters that I really struggled with. The letter “h” was the hardest for me and to this day still is. The opening phrase at the San Antonio Express News was: “Thank you for calling the San Antonio Express News, this is Mark, how can I help you?” Two “h” words! So, I changed this to: “Thank you for calling the San Antonio Express News, this is Mark, what can I do for you?” A simple change but this really helped me on the phones.
Despite my speech issues, I never got any complaints or questions from customers or co-workers who couldn’t understand me. I thought it would eventually go away, but it never did. It was getting more difficult every day for me to speak clearly and be understood and I was embarrassed.
On May 1, 2006, I saw Dr. Yvonne Page, a Speech Language Pathologist.
As I soon started talking, Dr. Page knew exactly what I had. She asked me a lot of questions trying to pinpoint my problems and took a lot of notes. She eventually had me read these phrases: “Early one morning, a man and a woman were ambling along a 1-mile lane, running near Rainy Island Avenue” and "He saw half a shape mystically cross a simple path, at least 50 or 60 steps in front of his sister Kathy's house."
I read the first with ease but really struggled with the second sentence.
Dr. Page referred me to Dr. Blake Simpson, an Otolaryngologist, who works at the University of Texas Health Science Center. He would be able to get a better look at my vocal cords and verify my speech problems.
Dr. Simpson also wanted me to read those phrases. With the second phrase, it felt as if I forgot how to read. I couldn’t even say the word “house.” My mouth opened but nothing came out. It took a few seconds for the word “house” to finally come out and it didn’t sound good at all. By using a fiber optic Laryngoscopy, Dr. Simpson showed me what was happening with my vocal cords.
In May of 2006, I was officially diagnosed with a rare voice disorder called Abductor Spasmodic Dysphonia. According to the
Dysphonia website:
Spasmodic dysphonia (SD), a focal form of Dystonia, is a neurological voice disorder that involves involuntary "spasms" of the vocal cords causing interruptions of speech and affecting the voice quality. SD can cause the voice to break up or to have a tight, strained, or strangled quality. There is no cure. It is treatable by speech therapy and Botox injections in the vocal cords.
I started speech therapy with Dr. Page immediately after I was diagnosed. Our sessions were weekly for 12 weeks. For the first four weeks, we met twice a week. I was very lucky that my work schedule allowed me to have two consecutive days off during the week. Otherwise, I would have had to use all of my sick and vacation time.
We did a lot of breathing and relaxation exercises. We worked on the voiceless sounds. Every few weeks we would try words that began with the letter “h.” Dr. Page wanted me to have a soft voice; no yelling or talking loud on the phones. She had software that measured how loud my voice was and how much roughness I had. It was really interesting to see these changes before, during, and after a session. I was also able to hear my voice; it was good sometimes, bad sometimes, and sometimes just plain laughable!
I was relieved that the Speech Language Pathologist knew what I had as soon as I started talking. Unlike other people I have met with Spasmodic Dysphonia, I didn't have to wait months or years and see several other doctors to get the correct diagnosis. After lots of research, talking with Dr. Page and Dr. Simpson, and consulting with my parents, I decided to try the Botox injections. I was aware there could be side effects. But I was ready to take the plunge.
On August 14, 2006, I was in the waiting room at University Hospital in San Antonio, Texas. I was extremely nervous. My mother came with me and her support really helped me get thru the anticipation of getting my first Botox injection.
Dr. Simpson sprayed my nose to numb it. It didn't taste like anything, but it really made my nose runny!! He then inserted a needle into my neck to numb it. The numbing medication tasted really gross and made me cough a lot; but that means the numbing was working. A Neurologist, Dr. Carlayne Jackson, put some sensors on my stomach; this helps locate the proper spot for injection. A resident from the hospital was also in the room and he was the one who inserted the fiber optic Laryngoscope from my nose to my vocal cords.
I coughed a few times and said the letter "E" for a few seconds. I even read these phrases again “Early one morning, a man and a woman were ambling along a 1-mile lane, running near Rainy Island Avenue” and "He saw half a shape mystically cross a simple path, at least 50 or 60 steps in front of his sister Kathy's house."
Dr's. Simpson and Jackson located the correct spot for a unilateral injection and I didn't even feel the Botox. Wow! Afterwards, I was coughing a lot, had some discomfort in swallowing, and my voice was very strained. But, those side effects wore off quickly and I was very glad.
I went back for my 2nd Botox injection on October 23, 2006. I was more eager this time and was looking forward to how my voice would fare. It was the same procedure for the treatment. I had the same side effects but again they vanished quickly.
Since my diagnosis, I have had 17 Botox injections and I am getting fantastic results and do notice a HUGE difference in my voice. I always have the discomfort in swallowing, a strained voice, and lots of coughing. But, they go away quicker each time. My last 3 Botox injections have lasted about 6 months. I will probably schedule another Botox injection toward the end of the year. Each injection I get lasts longer than the previous.
If you heard me talk, you probably wouldn't even know I have any issues. I do struggle at work occasionally but nobody notices it. I am kinda curious to see how my voice would do without Botox?
At least I thought it was quiet...when I replayed it afterwards, I heard my keys jiggling and my turn signal clicking. Next time, I will unhook the car key from the miscellaneous keys and find a straight path to nowhere in particular. Other than that, I am very excited to debut my voice and hope you enjoy it.
This post was reproduced with permission from Mark at mdlblog.com.